Ultrasound Needle Guides: A Comprehensive Overview (Updated February 14, 2026)
Ultrasound needle guides enhance precision during procedures like biopsies and abscess drainage. The global market, per ResearchAndMarkets.com, is evolving with reusable and disposable options.
Ultrasound-guided needle procedures represent a significant advancement in medical intervention, offering real-time visualization during various diagnostic and therapeutic applications. This technique utilizes high-frequency sound waves to create images of structures beneath the skin, allowing clinicians to precisely guide needles to target areas.
Historically, procedures like biopsies and abscess drainages relied heavily on anatomical landmarks or fluoroscopic guidance. However, ultrasound provides a dynamic, radiation-free alternative. The ability to visualize the needle’s path in relation to surrounding tissues minimizes the risk of complications and improves accuracy.
The growing adoption of ultrasound needle guidance is driven by its versatility and accessibility. From core needle biopsies to fine needle aspirations, and even complex procedures like lung cancer staging (comparing EBUS-TBNA to TTNA), ultrasound is becoming increasingly integral to modern medical practice. This overview will delve into the core principles, types, applications, benefits, and future trends of this vital technology.
What is an Ultrasound Needle Guide?
An ultrasound needle guide is a specialized instrument designed to facilitate accurate needle placement during ultrasound-guided procedures. Essentially, it’s a device that attaches to the probe or is integrated with the ultrasound system, providing a pathway for the needle to enter the body.
These guides come in various designs, ranging from simple attachments to more sophisticated systems. A key feature is a mounting arrangement securing the guide body, ensuring stability during insertion. The guide helps maintain a consistent angle and depth, crucial for reaching the target lesion.
Needle guides are available in both reusable and disposable formats, catering to different clinical needs and infection control protocols. The selection of an appropriate guide depends on factors like needle gauge, procedure type, and operator preference. Ultimately, the goal is to enhance precision, reduce complications, and improve patient outcomes.
The Core Principles of Ultrasound-Guided Needle Procedures
Ultrasound-guided needle procedures rely on real-time visualization to navigate instruments with precision. High-frequency sound waves create images of internal structures, allowing operators to identify target lesions and avoid critical anatomy. This contrasts with blind techniques, significantly reducing the risk of complications.
A fundamental principle is the “in-plane” or “out-of-plane” approach, dictating the needle’s relationship to the ultrasound beam. Proper technique involves careful probe positioning, needle visualization throughout insertion, and continuous assessment of the surrounding tissues.
Understanding ultrasound physics – including resolution, depth, and artifacts – is crucial. Furthermore, meticulous attention to sterile technique and patient safety protocols is paramount. Ultrasound scanning is generally noninvasive and painless, but skilled operation is essential for maximizing benefits and minimizing potential risks.
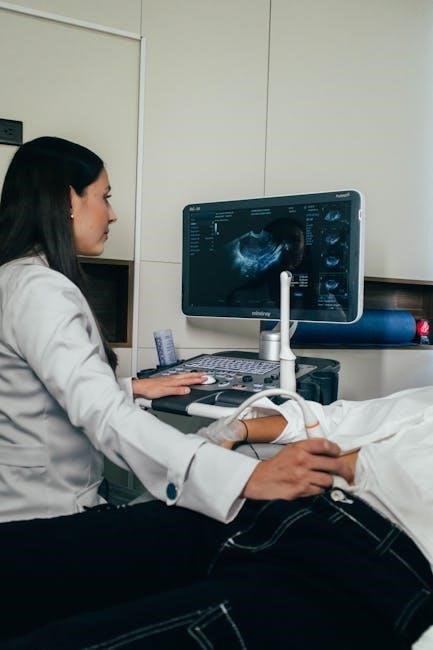
Types of Ultrasound Needle Guides
Ultrasound needle guides are categorized as reusable or disposable, impacting cost and sterility protocols. Needle gauge selection is critical for optimal sample acquisition and patient comfort.
Reusable vs. Disposable Needle Guides
Reusable ultrasound needle guides offer a cost-effective solution for facilities performing a high volume of procedures, though they necessitate rigorous sterilization protocols between each patient to prevent cross-contamination. These guides are typically constructed from durable materials designed for repeated use and cleaning. However, the thoroughness of sterilization is paramount and requires dedicated staff and quality control measures.
Disposable needle guides, conversely, eliminate the risk of cross-contamination and streamline workflow, reducing processing time and labor costs associated with sterilization. While the initial per-procedure cost is higher, the convenience and enhanced safety profile often outweigh this factor, particularly in settings where infection control is a top priority. The disposable segment currently holds the largest market share, reflecting this growing preference for single-use solutions.
The choice between reusable and disposable guides depends on a facility’s specific needs, budget, and infection control policies.

Needle Gauge and Selection
Needle gauge, a critical factor in ultrasound-guided procedures, directly impacts sample quality and patient comfort. A wider gauge needle (lower number) generally yields a larger core biopsy sample, beneficial for histological analysis, but can cause more discomfort and bleeding. Conversely, a smaller gauge needle (higher number) minimizes discomfort and complications but may provide insufficient material for accurate diagnosis.
The appropriate gauge depends on the target tissue, the required sample size, and the patient’s clinical condition. For fine needle aspiration biopsies (FNAB), smaller gauges are typically employed. Core needle biopsies often utilize 18-gauge needles, though variations exist. Careful consideration must be given to avoid sampling unrelated material, a potential issue with FNAB without ultrasound guidance.
Clinicians must balance diagnostic needs with patient well-being when selecting the optimal needle gauge for each specific case.
Specialized Guides for Different Procedures
Ultrasound needle guides aren’t one-size-fits-all; specialized designs cater to diverse procedures. For abscess drainage, guides facilitate precise needle placement into defined cavities, often under CT scan or ultrasound guidance, utilizing an 18-gauge introducer needle. Bronchoscopic procedures, like endobronchial ultrasound-guided transbronchial needle aspiration (EBUS-TBNA), require guides optimized for airway access.
Lung cancer diagnosis and staging benefit from guides designed for transthoracic needle aspiration (TTNA), offering alternatives to bronchoscopy. Biopsy procedures demand guides that ensure accurate targeting of lesions, minimizing off-target sampling. Atraumatic designs are increasingly favored to reduce tissue trauma and improve patient outcomes.
The mounting arrangement of a guide body is crucial for stability during insertion. Innovation focuses on adapting guide geometry to specific anatomical locations and procedural needs.

Applications of Ultrasound Needle Guides
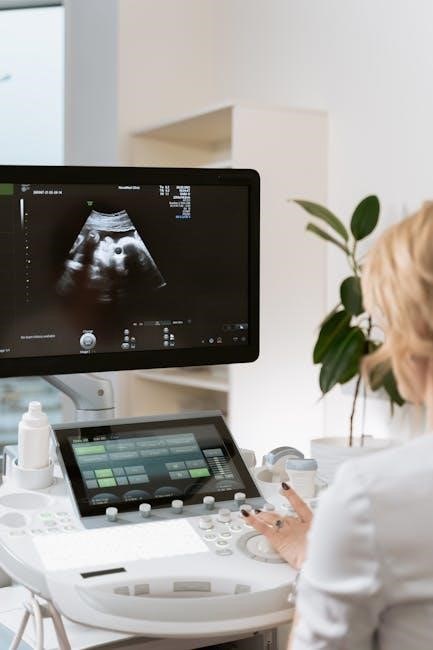
Ultrasound needle guides are vital for biopsies, abscess drainage, and lung cancer staging (EBUS-TBNA/TTNA). Fine needle aspiration biopsies (FNAB) also benefit from guided precision.
Biopsy Procedures with Ultrasound Guidance
Ultrasound guidance significantly improves the accuracy and safety of biopsy procedures across various specialties. Utilizing real-time imaging, clinicians can precisely target lesions and minimize the risk of sampling errors. Core needle biopsies benefit from guided insertion, ensuring representative tissue acquisition.
The availability of different needle gauges allows for tailored approaches based on the lesion’s characteristics and desired sample size. Ultrasound helps avoid critical structures, reducing potential complications. However, it’s crucial to acknowledge limitations; FNAB without guidance can yield non-specific samples.
Furthermore, ultrasound-guided biopsies are often less invasive than traditional surgical methods, leading to faster recovery times for patients. The use of specialized guides further enhances control during needle placement, contributing to more reliable diagnostic results. Proper technique remains paramount to minimize risks.
Abscess Drainage Guided by Ultrasound

Ultrasound guidance is a cornerstone of safe and effective abscess drainage. Real-time visualization allows clinicians to accurately identify the abscess cavity and guide the insertion of an 18-gauge introducer needle, minimizing the risk of damaging surrounding structures. This technique is particularly valuable for deep-seated or complex abscesses where palpation is unreliable.
Under ultrasound, CT scan, or fluoroscopic guidance, the needle is advanced into the defined cavity. Removing the trocar stylet then facilitates drainage. Ultrasound’s ability to differentiate between fluid and solid tissue is crucial for confirming correct needle placement.
Compared to blind drainage techniques, ultrasound guidance reduces the likelihood of incomplete drainage and recurrence. It also allows for assessment of the abscess’s size and complexity prior to intervention, aiding in treatment planning. Careful technique and adherence to sterile protocols are essential to prevent complications.
Lung Cancer Diagnosis & Staging (EBUS-TBNA vs. TTNA)
Ultrasound-guided needle techniques play a vital role in lung cancer diagnosis and staging, specifically comparing endobronchial ultrasound-guided transbronchial needle aspiration (EBUS-TBNA) with transthoracic needle aspiration (TTNA). EBUS-TBNA utilizes a bronchoscope with an ultrasound probe to visualize and access mediastinal lymph nodes and lung lesions from within the airways.
TTNA, conversely, involves needle insertion directly through the chest wall under imaging guidance – often CT scan, but ultrasound can be utilized for peripheral lesions. While EBUS-TBNA is less invasive, TTNA may be necessary for lesions inaccessible via bronchoscopy.
The choice between these methods depends on lesion location, size, and patient factors. Both techniques require precise needle guidance to obtain adequate tissue samples for accurate pathological assessment, crucial for determining cancer type and stage, ultimately guiding treatment decisions.
Fine Needle Aspiration Biopsy (FNAB) with Ultrasound
Ultrasound guidance significantly enhances the accuracy of Fine Needle Aspiration Biopsy (FNAB) procedures. Without ultrasound, FNAB can yield samples unrelated to the target lesion, particularly in challenging areas like salivary glands (SGs). Ultrasound allows real-time visualization of the needle’s path, ensuring precise targeting and maximizing the retrieval of representative cells.
This is particularly crucial for diagnosing superficial nodules and masses. The use of an ultrasound needle guide further stabilizes the needle, improving control and reducing the risk of sampling errors. Ultrasound also aids in identifying optimal access points and avoiding critical structures.
Consequently, ultrasound-guided FNAB leads to more reliable diagnoses, reducing the need for repeat biopsies and improving patient management. It’s a cornerstone of minimally invasive diagnostic procedures.
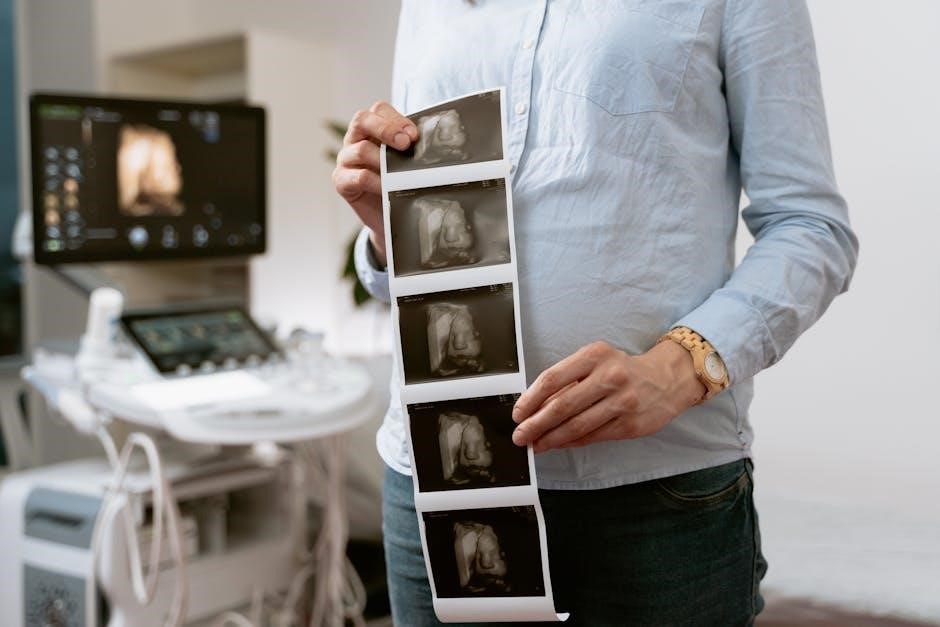
Benefits and Risks of Ultrasound Needle Guidance
Ultrasound scanning is largely noninvasive and typically painless, offering widespread availability. However, like any procedure, potential side effects and complications exist, requiring careful technique.
Benefits of Ultrasound Scanning
Ultrasound guidance offers a multitude of advantages in needle-based procedures. Most notably, it’s largely noninvasive, avoiding incisions and minimizing patient discomfort. Unlike methods relying on ionizing radiation like fluoroscopy or CT scans, ultrasound utilizes sound waves, presenting a safer alternative, particularly for repeated imaging.
Real-time visualization is a key benefit, allowing clinicians to directly observe the needle’s path and target tissue, enhancing accuracy and reducing the risk of hitting unintended structures. This is especially crucial in complex anatomical regions. Furthermore, ultrasound is widely accessible and relatively cost-effective compared to other imaging modalities.
The ability to differentiate between cystic and solid lesions is another significant advantage, guiding appropriate intervention. Improved sample acquisition, as seen in Fine Needle Aspiration Biopsy (FNAB), minimizes non-diagnostic results. Ultimately, ultrasound guidance contributes to increased procedural success rates and improved patient outcomes.
Potential Side Effects and Complications
While ultrasound-guided procedures are generally safe, potential side effects and complications exist. These can range from minor discomfort at the needle insertion site to more serious, though rare, events. Common, temporary effects include localized pain, bruising, and minor bleeding.
More significant complications, though infrequent, may involve infection, nerve damage, or injury to adjacent structures. The risk of these complications is heightened in procedures like abscess drainage or biopsies of deeper tissues. Inaccurate needle placement, even with ultrasound guidance, can lead to sampling of incorrect tissue or damage to vital organs.
FNAB, particularly without ultrasound, carries a higher risk of obtaining non-representative samples. Proper technique, meticulous attention to anatomical landmarks, and adherence to sterile protocols are crucial for minimizing these risks. Careful patient selection and informed consent are also essential components of safe practice.
Minimizing Risks with Proper Technique
Effective risk mitigation in ultrasound-guided needle procedures hinges on meticulous technique. Thorough patient assessment, including identifying contraindications, is paramount. Real-time visualization throughout the entire procedure – needle insertion, advancement, and sampling – is critical for accurate targeting and avoiding critical structures.
Employing appropriate needle gauge selection, based on the target tissue and procedure type, reduces trauma. Sterile technique, including skin preparation and sterile probe covers, minimizes infection risk. Utilizing atraumatic needle guide designs further enhances safety.
Post-procedure monitoring for signs of bleeding, infection, or nerve injury is essential. Operators should be proficient in managing potential complications. Continuous training and adherence to established guidelines are vital for maintaining competency and ensuring optimal patient outcomes. Proper technique significantly elevates the benefit-to-risk ratio.

Technological Advancements in Ultrasound Needle Guides
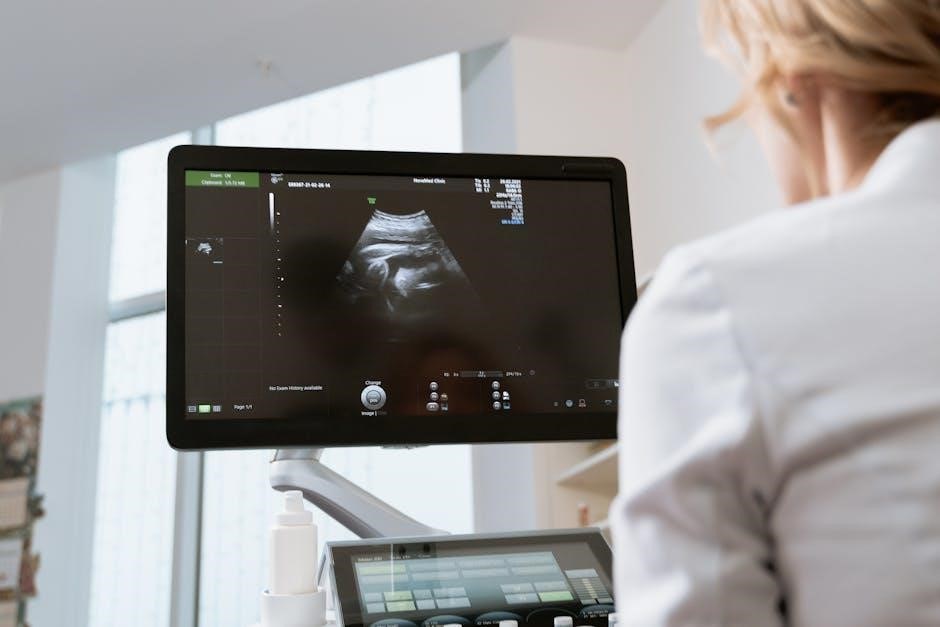
Innovations include integrating imaging technologies, developing atraumatic designs, and utilizing software like LEGO Education SPIKE Prime for enhanced precision during needle guidance.
Integration with Additional Imaging Technologies
Combining ultrasound guidance with other imaging modalities represents a significant advancement in procedural accuracy and safety. Historically, fluoroscopy and CT scans have been utilized for needle placement, offering distinct advantages in visualization, particularly for deep-seated targets. However, these methods involve ionizing radiation exposure.
The synergy between ultrasound and these technologies allows clinicians to leverage the real-time guidance of ultrasound with the anatomical detail provided by CT or the dynamic assessment of fluoroscopy. For instance, in lung procedures, endobronchial ultrasound-guided transbronchial needle aspiration (EBUS-TBNA) is often compared to transthoracic needle aspiration (TTNA), demonstrating the value of integrated approaches. This integration minimizes risks, improves target identification, and ultimately enhances diagnostic yield. Future developments will likely focus on seamless data fusion and augmented reality applications to further refine these combined imaging techniques.
Atraumatic Needle Guide Designs
Recent innovations in ultrasound needle guide technology prioritize minimizing patient trauma and discomfort. Traditional designs sometimes caused tissue distortion or unnecessary pain during insertion and manipulation. Atraumatic designs focus on smoother, more tapered guide profiles and specialized tip geometries to reduce resistance and displacement of surrounding structures.
These advancements often incorporate flexible materials and optimized needle trajectory control. The goal is to facilitate a more direct and less disruptive path for the needle, reducing the risk of collateral damage to nerves, vessels, and other sensitive tissues. Such designs are particularly crucial in procedures like fine needle aspiration biopsy (FNAB), where accurate sampling with minimal disturbance is paramount. Further research continues to explore bio-inspired designs and novel materials to achieve even greater levels of atraumatic performance, improving patient outcomes and procedural tolerance.
Software and Programming for Enhanced Precision (LEGO Education SPIKE Prime/Essential)
Emerging applications leverage programmable platforms like LEGO Education SPIKE Prime and Essential to refine ultrasound needle guidance. While seemingly unconventional, these systems offer a cost-effective method for prototyping and testing automated needle alignment and control algorithms.
Researchers are exploring using the SPIKE platform’s sensors and motors to create miniature robotic guides capable of precise needle positioning based on real-time ultrasound feedback. The intuitive programming interface allows for rapid iteration of control strategies, potentially enhancing accuracy and reducing operator dependence. This approach facilitates the development of customized solutions tailored to specific procedural needs. Furthermore, it provides a valuable educational tool for training medical professionals in advanced image-guided intervention techniques, bridging the gap between theoretical concepts and practical application.
Global Market Trends for Ultrasound Needle Guides
The ultrasound needle guide market is experiencing growth, with disposable guides dominating. A ResearchAndMarkets.com report highlights regional analysis and future innovations driving expansion.
Market Overview and Growth (ResearchAndMarkets.com Report)
The global ultrasound needle guides market, as detailed in the ResearchAndMarkets.com report published April 29, 2025, demonstrates a positive trajectory. This growth is fueled by increasing demand for minimally invasive procedures, rising prevalence of chronic diseases requiring image-guided interventions, and technological advancements in ultrasound technology itself.
The report segments the market by type, identifying disposable needle guides as currently holding the largest share due to concerns regarding sterilization and infection control. However, reusable options remain relevant, particularly in settings with robust sterilization protocols. Geographic analysis reveals varying adoption rates, with North America and Europe currently leading the market, followed by Asia-Pacific, which is expected to exhibit the highest growth rate due to expanding healthcare infrastructure and increasing patient awareness.
Key players are focusing on innovation, including integration with other imaging modalities and the development of atraumatic designs. The overall market is poised for continued expansion, driven by the benefits of increased accuracy, reduced complications, and improved patient outcomes associated with ultrasound-guided procedures.
Regional Market Analysis
North America currently dominates the ultrasound needle guide market, benefiting from well-established healthcare systems, high adoption rates of advanced imaging technologies, and a large volume of interventional procedures. Europe follows closely, driven by similar factors and supportive government healthcare initiatives.
However, the Asia-Pacific region is projected to experience the most significant growth. This surge is attributed to rapidly expanding healthcare infrastructure, increasing disposable incomes enabling greater access to advanced medical care, and a rising prevalence of chronic diseases necessitating image-guided interventions. Countries like China and India are key contributors to this growth.
Latin America and the Middle East & Africa represent emerging markets with moderate growth potential. Factors influencing growth in these regions include increasing healthcare expenditure, improving healthcare access, and a growing awareness of the benefits of ultrasound-guided procedures. Market penetration is, however, currently limited by economic constraints and infrastructure challenges.
Future Projections and Innovations
The ultrasound needle guide market is poised for continued expansion, driven by technological advancements and increasing clinical demand. Integration with additional imaging technologies, such as CT and MRI, will enhance precision and broaden application scope. Atraumatic needle guide designs are gaining traction, minimizing patient discomfort and tissue damage.
Software and programming, exemplified by platforms like LEGO Education SPIKE Prime/Essential, are enabling the development of more sophisticated and customizable guidance systems. Expect increased automation and real-time image processing capabilities. Further innovation will focus on reducing guide size and improving visualization.
Future projections indicate a shift towards personalized medicine, with guides tailored to specific patient anatomy and procedure requirements. Artificial intelligence (AI) integration will likely play a crucial role in optimizing needle trajectory and enhancing diagnostic accuracy, ultimately improving patient outcomes and expanding the market’s reach.
Leave a Reply
You must be logged in to post a comment.